
Famous People
 FATHER OF THE LOBOTOMY
FATHER OF THE LOBOTOMY
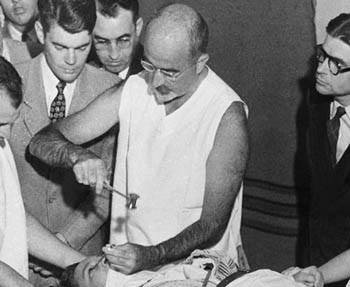
Thinking of giving someone a piece of your mind? Steer clear of this guy.
by John McManamy

Thinking of giving someone a piece of your mind? Steer clear of this guy.
by John McManamy
THE FIELD OF MENTAL HEALTH suffers no shortage of weird and offbeat and arguably despicable characters, but the Washington Post back in the early 2000s outdid itself for its story on Walter Freeman, father of the lobotomy. Sample this lurid paragraph for starters:
Walter Freeman lifted the patient's eyelid and inserted an ice pick-like instrument called a leucotome through a tear duct. A few taps with a surgical hammer breached the bone. Freeman took a position behind the patient's head, pushed the leucotome about an inch and a half into the frontal lobe of the patient's brain, and moved the sharp tip back and forth. Then he repeated the process with the other eye socket.
Freeman kept records of 3,439 lobotomies he performed over his long career, and he promoted the procedure to more than 55 hospitals in 23 states. At AMA meetings, he set up graphic exhibits and used hand-held clackers to draw audiences.
In all, lobotomies were used on 40,000 to 50,000 Americans between 1936 and the late 1950s. Freeman believed lobotomies worked because the procedure severed connections between the frontal lobes of the brain and the thalamus, thought to be the seat of human emotion, which the mentally ill apparently had in overabundance. Although his theories have been discredited, Freeman was one of the few psychiatrists of his era who believed that mental illness had a physical biological component.
Freeman attended Yale and the University of Pennsylvania School of Medicine, then studied neurology and psychiatry in Europe. Motivated by the tragedy of wasted lives in mental hospitals, he introduced insulin shock therapy and ECT for patients at George Washington University Hospital in Washington DC, where he served on the faculty. He also had a private practice and was director of the laboratories at St Elizabeth's Hospital.
SIGN UP FOR MY FREE EMAIL NEWSLETTER
Upon finding out that chimpanzees became subdued when their frontal lobes were damaged, and spurred into action by Portuguese neurologist Egas Moniz' experiments on people, he and colleague James Watts started practicing on brains from the hospital morgue, and in 1936 they were ready for their first patient, a Mrs Hammatt, 63, who suffered from agitated depression and sleeplessness. The technique of entering the frontal lobes through the eye sockets was still far off into the future. Instead, they drilled six holes into the top of her skull.
According to Freeman, Mrs Hammet emerged transformed, able to "go to the theatre and really enjoy the play ... " She lived another five years.
Freeman and Watts claimed 52 percent of their first 623 surgeries yielded "good" results, but they did not offer a clinical yardstick for what constituted an improvement. Patients often had to be retaught how to eat and use the bathroom. Relapses were common, and three percent died from the procedure. The most famous Freeman-Watts failure was JFK's sister, Rosemary Kennedy, who needed full-time care for 64 years (she died in Jan 2005).
Nevertheless, hospitals were willing to put up with lobotomies and all their shortcomings for no other apparent reason than post-operation lethargic patients were easier to handle than pre-operation emotionally charged ones.
In 1967, Freeman performed a lobotomy on one of his original patients in Berkeley, California. He severed a blood vessel, and the patient died three days later. This effectively brought his career full circle. During the last five years of his life, he performed no more lobotomies. He died from cancer in 1972, age 76.
The Washington Post reported there are probably fewer than 20 brain operations a year (not lobotomies) in the US to treat psychiatric disorders, part of the negative legacy of Freeman that has scared away researchers and funders.
In 2008, the FDA approved deep brain stimulation (DBS) for OCD, and the surgery is being investigated for depression. The surgery, which was developed for treating Parkinsons, involves inserting an electronic lead into the folds of the brain. Unlike lobotomies and surgeries such as capsulotomies, no surgical incisions are made. Nothing is severed. DBS for psychiatric illness is extremely rare and is used as a last resort.
In 1949, at Freeman’s urging, Moniz received the Nobel Prize. As Nassir Ghaemi MD of Tufts University in a review commented:
It is quite ironic that in that same year, the Australian psychiatrist John Cade would discover lithium ... yet after the Moniz fiasco, the Nobel committee apparently has shied away from giving awards for direct treatment of mental illness, and thus the discoverers of lithium, antipsychotics, and antidepressants have never been duly recognized.
One day that may change. But first the ghost of Freeman needs to be thoroughly lobotomized.
Reviewed July 15, 2016
NEW!
Follow me on the road. Check out my New Heart, New Start blog.
 MORE ARTICLES ON McMAN
MORE ARTICLES ON McMAN
 FEATURED VIDEOS
FEATURED VIDEOS









